Around 788 million people worldwide are living with Chronic Kidney Disease — and most don't even know it. CKD is a silent epidemic that advances without symptoms in its early stages, irreversibly destroys kidney function, and is already the 9th leading cause of death on the planet. In Brazil alone, more than 172,000 people depend on dialysis to survive, and the numbers are growing by nearly 10% per year. This guide brings together everything you need to know: from the first warning signs to the most advanced treatments of 2025, along with alarming data that reveals why this disease demands your urgent attention.
What Is Chronic Kidney Disease (CKD)?
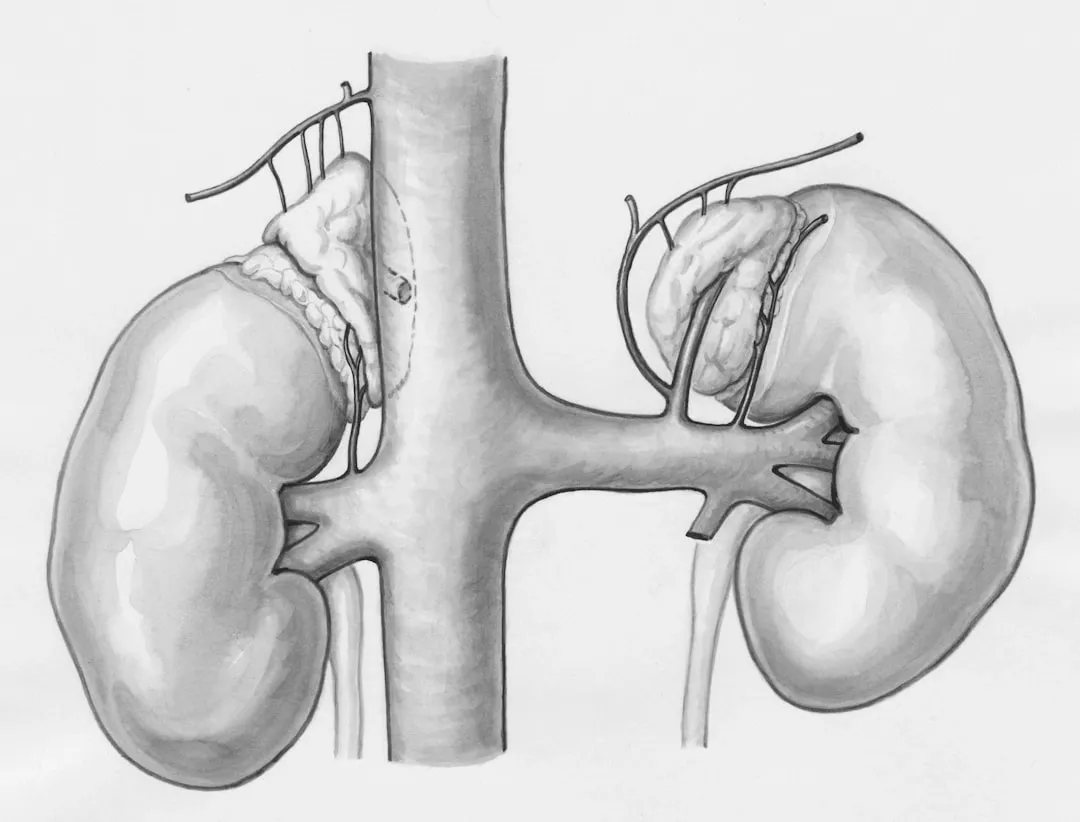
The kidneys are vital organs that filter approximately 180 liters of blood per day.
Chronic Kidney Disease (CKD), also known as chronic renal failure, is a progressive and irreversible condition in which the kidneys gradually lose their ability to filter blood, eliminate toxins, and regulate the body's fluid and electrolyte balance.
The official diagnosis of CKD follows clearly defined criteria from KDIGO (Kidney Disease: Improving Global Outcomes):
- Estimated Glomerular Filtration Rate (eGFR) below 60 mL/min/1.73 m² for more than 3 months, OR
- Presence of kidney damage (such as albuminuria, imaging abnormalities, or biopsy findings) for more than 3 months, regardless of eGFR.
Kidneys are extraordinary organs. About the size of a fist, each kidney contains approximately 1 million nephrons — microscopic units responsible for filtering about 180 liters of blood per day. When these nephrons are progressively destroyed, the body begins to accumulate toxic waste, excess fluids, and imbalanced electrolytes, generating a cascade effect that compromises virtually every system in the body.
The great tragedy of CKD lies in its silent nature. In the early stages, the body compensates for kidney loss by overloading the remaining nephrons, meaning the patient may feel absolutely nothing while losing up to 70% of kidney function. When symptoms finally appear, the damage is usually extensive and irreparable.
A Silent Pandemic: Alarming Global Numbers
The Worldwide Picture
Data from the latest Global Burden of Disease (GBD) 2023 study, published in The Lancet, reveals the frightening magnitude of the problem:
| Indicator | Value |
|---|---|
| People with CKD worldwide (2023) | 788 million (adults ≥20 years) |
| Global age-standardized prevalence | 14.2% |
| Ranking among causes of death | 9th cause (1.48 million deaths/year) |
| Growth since 1990 | from 378 million to 788 million (+108%) |
| Projection for 2040 | 5th leading cause of years of life lost |
| Contribution to cardiovascular deaths | ~12% of global CV deaths |
These numbers place CKD as one of the fastest-growing non-communicable diseases on the planet. Prevalence has more than doubled in three decades, driven by population aging and the explosion of diabetes, hypertension, and obesity.
Regional Disparities: Who Suffers Most?
The burden of CKD is not evenly distributed across the globe. The most affected regions in 2023 were:
| Region | Age-Standardized Prevalence |
|---|---|
| North Africa and Middle East | 18.0% |
| South Asia | 15.8% |
| Sub-Saharan Africa | 15.6% |
| Latin America and Caribbean | 15.4% |
| East Asia | ~13% |
| Western Europe | ~11% |
These disparities reflect differences in access to primary health care, prevalence of metabolic risk factors, and socioeconomic conditions that hinder early diagnosis. In low- and middle-income countries, fewer than 5% of patients with end-stage CKD gain access to dialysis treatment, in contrast to developed countries where coverage reaches nearly 100%.
The Brazilian Portrait: A Humanitarian Crisis in Progress
Prevalence and Impact in Brazil
Brazil faces a particularly concerning scenario. According to the Brazilian Society of Nephrology (SBN) and the Ministry of Health:
- CKD affects between 10.5% and 14% of the general population in Brazil
- In at-risk groups (diabetics and hypertensives), prevalence reaches 36%
- Between 2019 and 2023, there was a 152.81% increase in CKD consultations in Primary Health Care (PHC)
Brazilian Dialysis Census 2024
The 2024 SBN Census brought data that triggered maximum alert in the nephrology community:
| Indicator (Brazil, 2024) | Data |
|---|---|
| Patients on dialysis | 172,585 |
| Increase vs. 2023 | ~10% |
| New patients in the year | 52,944 |
| Hemodialysis | 87.3% of patients |
| Peritoneal dialysis | 5.6% |
| Hemodiafiltration | 7.1% |
| Gross annual mortality rate | 16.5% |
| SUS financing | ~80% of treatments |
| SUS investment (2023) | R$4 billion (~US$800 million) |
The most alarming finding is that the age group over 65 is the fastest growing among dialysis patients, and 59% are male. The SBN has classified the situation as a "dialysis humanitarian crisis", pointing to chronic underfunding of the sector as a real threat to the lives of thousands of Brazilians.
Why Is This Happening in Brazil?
The convergence of several factors fuels this crisis:
- Epidemiological transition: Brazil rapidly shifted from a profile of infectious diseases to chronic diseases, without the health system adapting at the same pace.
- Diabetes and hypertension epidemic: These two conditions account for more than 60% of CKD cases in the country.
- Rising obesity: More than 60% of Brazilian adults are overweight or obese.
- Inequality in access: Northern and Northeastern regions have significantly fewer nephrologists and dialysis clinics per capita.
- Late diagnosis: Most patients reach the nephrologist already at an advanced stage, when dialysis is unavoidable.
The 5 Stages of CKD: Understanding the Progression
The classification of CKD into 5 stages, based on the Glomerular Filtration Rate (GFR), is essential for guiding treatment and prognosis. Understanding each phase enables earlier and more effective interventions.
Stage 1 — Kidney Damage with Preserved Function
GFR ≥ 90 mL/min/1.73 m²
The kidneys still filter blood normally, but signs of damage already exist — such as protein in the urine (albuminuria) or structural changes detectable by imaging tests. The patient feels absolutely nothing. This is the golden window for intervention, but it is rarely diagnosed without routine testing.
What to do: Rigorously control diabetes and blood pressure. Lifestyle changes can stabilize or even reverse damage at this stage.
Stage 2 — Mild Loss of Function
GFR between 60 and 89 mL/min/1.73 m²
Kidney function is mildly reduced, but the body still compensates. Symptoms remain absent in most cases. Detection depends on laboratory tests.
What to do: Begin regular monitoring, adjust medications, and adopt a specific diet if needed.
Stage 3 — Moderate Loss (Divided into 3a and 3b)
Stage 3a — GFR between 45 and 59 mL/min/1.73 m²
The first subtle signs appear: mild fatigue, subtle swelling, changes in urine color and frequency. Anemia and bone disease may begin to manifest. This is the stage at which many patients are first diagnosed.
Stage 3b — GFR between 30 and 44 mL/min/1.73 m²
Symptoms become more evident: pronounced anemia, bone pain, difficulty concentrating, loss of appetite, and general malaise. Metabolic complications require specific treatment.
What to do: Mandatory follow-up with a nephrologist. Strict dietary adjustments (restriction of potassium, phosphorus, and sodium). Treatment of anemia with erythropoietin and iron.
Stage 4 — Severe Loss (Pre-Dialytic Phase)
GFR between 15 and 29 mL/min/1.73 m²
This is the critical stage. The accumulation of toxins in the blood (uremia) causes significant symptoms: constant nausea, vomiting, weight loss, shortness of breath, extreme fatigue, edema, malnutrition, bone weakening, intense itching, and severe cardiovascular complications such as arrhythmias.
What to do: Preparation for renal replacement therapy (dialysis or transplant). Creation of arteriovenous fistula (for hemodialysis) or placement of peritoneal catheter. Evaluation for kidney transplant.
Stage 5 — Kidney Failure (End-Stage Renal Disease)
GFR < 15 mL/min/1.73 m²
The kidneys can no longer maintain vital functions. Without treatment, this stage is incompatible with life. Symptoms include mental confusion, uncontrollable vomiting, extreme weakness, massive fluid accumulation, and imminent risk of cardiac arrest from hyperkalemia.
What to do: Immediate initiation of dialysis or kidney transplant. This is a medical emergency when diagnosed for the first time.
The Silent Disease: Signs and Symptoms You Must Not Ignore
CKD is often called the "silent killer" because it can destroy up to 70-80% of kidney capacity before producing noticeable symptoms. When signs finally appear, they usually indicate the disease is already at stages 3b to 5.
Early Warning Signs (Frequently Ignored)
- Foamy or bubbly urine: indicates protein in the urine (proteinuria)
- Changes in urinary frequency: urinating more often at night (nocturia) or reduced urine volume
- Disproportionate fatigue: tiredness that doesn't improve with rest, caused by anemia
- Puffiness around the eyes upon waking: a sign of fluid and protein retention
- Swelling in ankles and feet: fluid accumulation due to impaired filtration
- Hard-to-control blood pressure: hypertension that doesn't respond well to medications
Advanced Stage Symptoms
- Nausea, vomiting, and complete loss of appetite
- Intense and persistent itching (uremic pruritus)
- Shortness of breath and breathing difficulty
- Muscle cramps and spasms
- Mental confusion, disorientation, and difficulty concentrating
- Metallic or ammonia-like breath (uremic breath)
- Chest pain (pericardial effusion)
- Involuntary weight loss
- Dry, yellowish, or grayish skin
- Blood in the urine (hematuria)
Warning: If you have two or more of these symptoms, especially if you are diabetic, hypertensive, or over 60, see a nephrologist immediately. A simple blood test (creatinine) and urine test (albumin-to-creatinine ratio) could save your life.
Why Do Kidneys Fail? Risk Factors and Causes
Primary Causes (Responsible for ~70% of Cases)
1. Diabetes Mellitus (Type 1 and Type 2)
Diabetes is the leading cause of CKD worldwide. Chronic hyperglycemia damages the renal glomeruli, causing diabetic nephropathy. Approximately 30-40% of diabetics develop CKD over their lifetime. Strict glycemic control (HbA1c < 7%) can significantly delay progression.
2. Systemic Arterial Hypertension (SAH)
High blood pressure is the second leading cause of CKD and is present in more than 85% of patients at advanced stages. SAH damages renal blood vessels, reducing flow and filtration capacity. The blood pressure target for CKD patients is < 130/80 mmHg, according to the KDIGO 2024 guidelines.
Other Important Causes
- Glomerulonephritis: Inflammatory diseases of the glomeruli, including IgA nephropathy, membranous and lupus glomerulonephritis
- Polycystic kidney disease: Genetic cause with formation of multiple cysts in the kidneys
- Chronic urinary obstruction: Recurrent kidney stones, prostatic hyperplasia, tumors
- Interstitial nephritis: Caused by medications (NSAIDs, nephrotoxic antibiotics), infections, or autoimmune diseases
- Chronic NSAID use: Ibuprofen, diclofenac, and naproxen used without prescription are preventable and frequent causes
- Obesity: Elevated BMI is an independent risk factor that increases glomerular hyperfiltration
Non-Modifiable Risk Factors
- Age: Risk increases significantly after 60
- Sex: Prevalence is slightly higher in women, but men progress more rapidly
- Family history: Having first-degree relatives with CKD doubles the risk
- Ethnicity: Black, Indigenous, and Hispanic populations show greater predisposition
- Low birth weight: Associated with fewer nephrons from birth
Modifiable Risk Factors
- Smoking (reduces renal blood flow)
- Sedentary lifestyle
- Diet high in sodium, refined sugar, and excessive animal protein
- Chronic dehydration
- Indiscriminate use of non-prescription medications
Diagnosis: How to Discover CKD Before It's Too Late

Early diagnosis of CKD can save lives — simple blood and urine tests are sufficient.
Early detection is the most important pillar in the fight against CKD. Three simple and accessible tests can identify the disease in its early stages:
1. Serum Creatinine and eGFR
Creatinine is a waste product of muscle activity filtered by the kidneys. When the kidneys fail, its blood levels rise. From creatinine, the eGFR is calculated, estimating how many milliliters of blood the kidneys filter per minute. The KDIGO 2024 guideline recommends the combined use of creatinine and cystatin C (eGFRcr-cys) for greater accuracy, and has eliminated the use of race in the calculation.
2. Urinary Albumin-to-Creatinine Ratio (uACR)
Detects the presence of albumin in the urine — an early marker of kidney damage that can be elevated even when eGFR is still normal. The classification is:
| Category | Value (mg/g) | Meaning |
|---|---|---|
| A1 | < 30 | Normal to mildly increased |
| A2 | 30-300 | Moderately increased (microalbuminuria) |
| A3 | > 300 | Severely increased (macroalbuminuria) |
3. Complementary Tests
- Renal ultrasound (assessment of size, cysts, and obstruction)
- Complete blood count (identification of anemia)
- Calcium, phosphorus, and PTH (assessment of bone disease)
- Serum electrolytes (sodium, potassium, bicarbonate)
- Lipid profile and blood glucose/HbA1c
Who Should Be Screened Annually?
KDIGO 2024 recommends annual screening for:
- Type 1 and Type 2 diabetics
- Hypertensives
- People over 60 years old
- Obese individuals (BMI ≥ 30)
- Patients with cardiovascular disease
- First-degree relatives of CKD patients
- People with chronic use of nephrotoxic medications
Treatment: From Conservative to Transplant

A balanced diet is a fundamental part of conservative CKD treatment.
Conservative Treatment (Stages 1-3)
The goal is to delay progression as much as possible and preserve remaining kidney function:
Blood pressure control:
- Target: < 130/80 mmHg
- First-line drugs: ACE inhibitors (enalapril, ramipril) or angiotensin receptor blockers (losartan, valsartan), which have nephroprotective effects
Glycemic control:
- HbA1c target: < 7% (individualized)
- Metformin use down to eGFR > 30 mL/min
- SGLT2 inhibitors (dapagliflozin, empagliflozin): revolutionized treatment by demonstrating up to 39% reduction in CKD progression, regardless of whether the patient has diabetes
Nutritional management:
- Sodium restriction (< 2,000 mg/day)
- Protein: 0.6 to 0.8 g/kg/day in stages 3-5 (pre-dialysis)
- Potassium and phosphorus control according to stage
- DASH and Mediterranean diets are recommended
Management of complications:
- Anemia: recombinant erythropoietin + intravenous iron supplementation
- Mineral bone disease: active vitamin D (calcitriol), phosphate binders
- Metabolic acidosis: oral sodium bicarbonate
- Dyslipidemia: statins
Dialysis (Stage 5 or Refractory Symptoms in Stage 4)
When the kidneys can no longer sustain life, dialysis artificially assumes the blood-filtering function:
Hemodialysis (87.3% of patients in Brazil):
- Performed 3 times a week, for 3 to 4 hours per session
- Blood is pumped through a machine with filters (dialyzers)
- Requires vascular access: arteriovenous fistula (ideal) or catheter
- Performed in specialized clinics
Peritoneal Dialysis (5.6% of patients in Brazil):
- Uses the peritoneum (abdominal lining) as a natural filter
- Can be done at home, daily
- Types: CAPD (manual, 4 exchanges/day) or APD (automated, overnight)
- Offers more autonomy and flexibility for the patient
Kidney Transplant
Considered the "gold standard" for end-stage renal disease, transplant offers better quality of life and greater survival compared to dialysis:
- Can come from a living (related or unrelated) or deceased donor
- Average waiting time in Brazil: 3 to 5 years on the SUS (public health system) list
- Brazil has the 2nd largest kidney transplant program in the world (behind only the US)
- Requires continuous immunosuppressant use to prevent rejection
Revolutionary Advances: What's New in 2025
Nephrology is experiencing a period of unprecedented transformation. The most significant advances include:
1. SGLT2 Inhibitors — The Biggest Revolution in Decades
Originally developed for diabetes, SGLT2 inhibitors (dapagliflozin and empagliflozin) have demonstrated impressive benefits for all CKD patients, with or without diabetes:
- 39% reduction in the risk of progression to kidney failure
- Reduction in cardiovascular events
- KDIGO 2024 guidelines recommend SGLT2i for every CKD patient with eGFR ≥ 20 mL/min
2. Semaglutide (Ozempic) for Kidney Protection
In 2025, semaglutide — the well-known GLP-1 receptor agonist already used for diabetes and obesity — received approval for kidney protection in adults with type 2 diabetes and CKD. Studies showed significant reduction in kidney function loss and cardiovascular events.
3. New Medications for Glomerulopathies
- Atrasentan: Accelerated FDA approval for IgA nephropathy, with significant reduction in proteinuria
- Iptacopan and Pegcetacoplan: Approved in 2025 for C3 glomerulopathy, a rare kidney disease
- Fabhalta, Vanrafia, and Voyxact: New medications targeting specific mechanisms of kidney damage
4. Xenotransplantation — Pig Kidneys in Humans
In 2025, clinical trials were approved to transplant genetically modified pig kidneys into patients with kidney failure. This historic advance could, in the future, eliminate the organ shortage that condemns thousands to the waiting list.
5. Artificial Intelligence in Nephrology
AI and machine learning models are rapidly advancing in their ability to predict CKD progression to end-stage renal disease, enabling earlier interventions and personalized management. Non-invasive tests using AI and retinal scanning are being developed for CKD risk prediction.
6. Post-Transplant Immunosuppressant Reduction
Research in 2025 showed promising results in combined kidney and stem cell transplants, with the potential to reduce or eliminate the need for lifelong immunosuppressive medications.
Prevention: 12 Measures That Protect Your Kidneys

Regular physical exercise is one of the most effective measures to protect kidney health.
Prevention is the most powerful weapon against CKD. Studies show that up to 50% of cases could be prevented or significantly delayed with simple measures:
1. Strict Diabetes Control
Keep HbA1c below 7%. Diabetic nephropathy is the leading cause of CKD.
2. Monitor Your Blood Pressure
Target: < 130/80 mmHg. Silent hypertension is a kidney killer.
3. Maintain a Healthy Weight
BMI between 18.5 and 24.9. Obesity causes hyperfiltration and glomerular damage.
4. Exercise Regularly
Minimum 150 minutes per week of moderate aerobic activity (walking, swimming, cycling) + 2 days of muscle strengthening.
5. Adopt a Protective Diet
DASH or Mediterranean diet: rich in fruits, vegetables, whole grains. Limit sodium (< 2,300 mg/day), refined sugar, and red meat.
6. Stay Adequately Hydrated
Drink at least 2 liters of water per day (adjust according to CKD stage and medical guidance).
7. Quit Smoking
Smoking reduces renal blood flow by up to 20% and accelerates fibrosis.
8. Avoid Non-Prescribed Anti-Inflammatories
NSAIDs (ibuprofen, diclofenac) are nephrotoxic. Never use them chronically without medical guidance.
9. Moderate Alcohol
Excessive consumption causes dehydration and overworks the kidneys.
10. Get Annual Tests
Serum creatinine and urinary albumin-to-creatinine ratio: two affordable tests that can detect CKD years before symptoms.
11. Control Cholesterol
Dyslipidemia contributes to vascular and renal damage.
12. Treat Urinary Infections Promptly
Recurrent infections can cause cumulative kidney damage, especially in women.
Cardiovascular-Kidney-Metabolic (CKM) Syndrome: The New Paradigm
One of the most important concepts in modern medicine is the recognition that heart, kidneys, and metabolism function as an integrated system. CKM Syndrome, formalized by the American Heart Association, recognizes that:
- Kidney disease increases by 5 times the risk of heart attack and stroke
- Heart failure accelerates renal deterioration
- Diabetes and obesity fuel both cardiac and renal disease
- ~12% of all cardiovascular deaths worldwide are attributable to kidney dysfunction
This integrated view has fundamentally changed the therapeutic approach: it's not enough to treat the kidneys in isolation. Multidisciplinary care involving nephrologist, cardiologist, endocrinologist, nutritionist, and physical educator is required.
Living with CKD: Quality of Life Is Possible

Staying hydrated is essential for those living with chronic kidney disease.
Receiving a CKD diagnosis can be devastating, but millions of people live full and productive lives with the disease when it is properly managed:
Emotional Health
- Anxiety and depression affect up to 40% of CKD patients
- Psychological support should be part of the treatment
- Patient support groups and associations provide valuable support
Physical Activity
- Exercise is safe and recommended at all stages, including during dialysis
- Walking, yoga, swimming, and light resistance exercises are the most recommended
- Intradialytic exercise (during hemodialysis sessions) significantly improves quality of life
Nutrition
- Working with a specialized dietitian is essential
- Recipes adapted for potassium, phosphorus, and sodium restrictions can be tasty and nutritious
- Apps like "MyFitnessPal" and "Kidney Kitchen" help with dietary management
Work and Social Life
- Most patients in stages 1-3 maintain normal professional activity
- Dialysis patients have specific labor rights in Brazil (flexible schedules for treatment)
- Home peritoneal dialysis offers more flexibility for working individuals
What the Public Needs to Know: Key Messages
CKD is silent. You can lose 70% of kidney function without feeling anything. Regular tests are the only protection.
Diabetes and high blood pressure are the main culprits. If you have either condition, monitor your kidneys annually.
Effective treatments exist. SGLT2 inhibitors have revolutionized nephrology and can delay progression by decades.
Prevention works. Up to half of cases can be prevented with a healthy lifestyle.
Diagnosis is not a death sentence. With proper treatment, millions of people live well with CKD.
Brazil has one of the largest transplant programs in the world. The SUS (public health system) offers dialysis, transplant, and medications free of charge.
Non-prescription anti-inflammatories destroy kidneys. Never use ibuprofen or diclofenac chronically.
Kidney disease kills the heart. 12% of cardiovascular deaths are caused by kidney problems.
Sources and References
- GBD 2023 CKD Collaborators. Global, regional, and national burden of chronic kidney disease, 1990–2023. The Lancet, 2025.
- KDIGO 2024. Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease. Kidney International, 2024.
- Brazilian Society of Nephrology (SBN). Brazilian Dialysis Census 2024. Brazilian Journal of Nephrology, 2024.
- Brazilian Ministry of Health. Clinical Guidelines for CKD Patient Care in SUS. Brasília, 2024.
- National Kidney Foundation (NKF). KDOQI Clinical Practice Guidelines for CKD. 2024.
- American Kidney Fund. Kidney Disease Statistics and Research Updates, 2025.
- Mayo Clinic. Chronic Kidney Disease — Symptoms and Causes. 2024.
- MSD Manuals. Chronic Kidney Disease (CKD). 2024.
- Centers for Disease Control and Prevention (CDC). Chronic Kidney Disease in the United States. 2024.
- American Diabetes Association. Standards of Care in Diabetes — Chronic Kidney Disease. Diabetes Care, 2025.
- World Health Organization (WHO). Kidney Disease: Facts and Figures. 2024.
This article is for informational and educational purposes only. It does not replace consultation with a qualified healthcare professional. If you suspect you have CKD or have risk factors, seek a nephrologist.





