In March 2026, Brazil is once again in the spotlight of global public health. With 140 confirmed Mpox cases, over 500 suspected cases under investigation, and the discovery of a new recombinant variant combining clades Ib and IIb, the country leads worldwide searches for the topic. But what does this really mean? Are we facing a new pandemic? What is the real risk to the population?
In this comprehensive article, we will break down the Mpox situation in Brazil and worldwide in 2026, explain what changed since the 2022 outbreak, analyze the new recombinant variant, and provide practical information about prevention, symptoms, and treatment based on the most reliable sources available.
What is Mpox? A Brief History
Mpox — previously known as "monkeypox" — is a viral zoonotic disease caused by the monkeypox virus, belonging to the same family as the smallpox virus (Poxviridae). Despite the former name, the main reservoir of the virus is not monkeys, but wild rodents in Central and West Africa.
The disease was first identified in humans in 1970 in the Democratic Republic of Congo, and for decades remained restricted to local outbreaks in Africa. Everything changed in May 2022, when an unprecedented outbreak spread across more than 100 countries, leading the World Health Organization (WHO) to declare an international public health emergency.
The Name Change
In November 2022, the WHO officially changed the name from "monkeypox" to "Mpox", addressing concerns about stigma and discrimination associated with the previous name. The change reflects a global trend toward medical nomenclature more sensitive to social implications.
Virus Clades
The Mpox virus is divided into two main clades, representing distinct genetic lineages with different clinical characteristics:
| Clade | Origin | Severity | Fatality Rate |
|---|---|---|---|
| Clade I (formerly "Congo Basin") | Central Africa | More severe | 1-10% |
| Clade II (formerly "West Africa") | West Africa | Less severe | <1% |
| Clade IIb | Mutation of Clade II | Mild to moderate | <0.1% |
| Clade Ib | Variant of Clade I | Moderate to severe | ~3% |
The 2022-2023 global outbreak was predominantly caused by Clade IIb, with low lethality. The concern in 2026 focuses on the emergence of more complex variants.
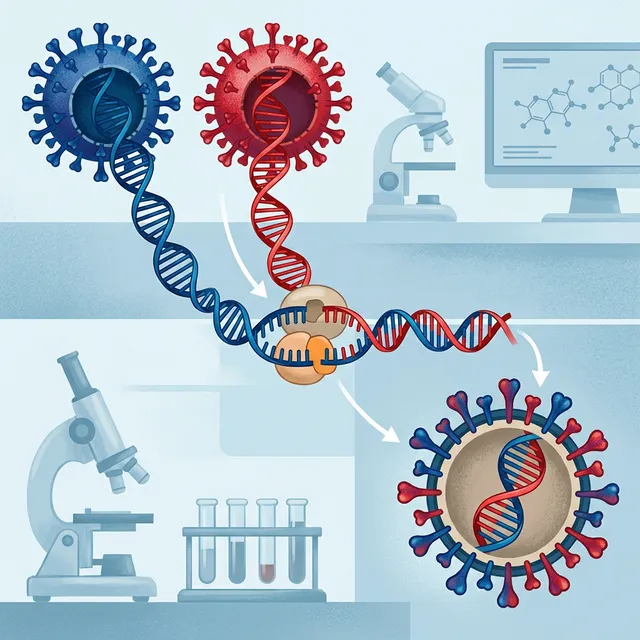
The New Recombinant Variant of 2026
In February 2026, the WHO documented an alarming discovery: a new recombinant strain of the Mpox virus combining genetic characteristics of clades Ib and IIb. This genetic recombination had never been observed before and represents a significant evolution of the virus.
What is a Recombinant Variant?
Viral recombination occurs when two different viruses infect the same host cell and exchange genetic material, resulting in a new variant carrying characteristics of both "parents." In the case of Mpox:
- From Clade Ib: the variant inherited potential for more severe cases, greater replication capacity, and possible immune evasion mechanisms.
- From Clade IIb: it inherited the high transmissibility that enabled the 2022 global outbreak, with adaptation to human-to-human transmission chains.
Where It Was Detected
The recombinant variant was first detected in the United Kingdom in December 2025. In January 2026, cases were confirmed in India. As of March 2026, the WHO monitors global spread, although no clinically severe cases have been specifically associated with this variant to date.
Why It Concerns Scientists
The concern of virologists is not based on current cases, but on evolutionary potential. A variant combining the severity of Clade I with the transmissibility of Clade II could, theoretically, represent a significantly more dangerous scenario than the 2022 outbreak. However, experts warn that recombination does not automatically mean increased danger — the virus may lose virulence while gaining transmissibility, or vice versa.
Brazil's Scenario in March 2026
Current Numbers
According to data from Brazil's Ministry of Health updated through March 9, 2026, the country recorded:
| Indicator | Number |
|---|---|
| Confirmed cases in 2026 | 140 |
| Suspected cases under investigation | 539-570 |
| Probable cases | 7-9 |
| Deaths | 0 |
| Cases in March | 11 |
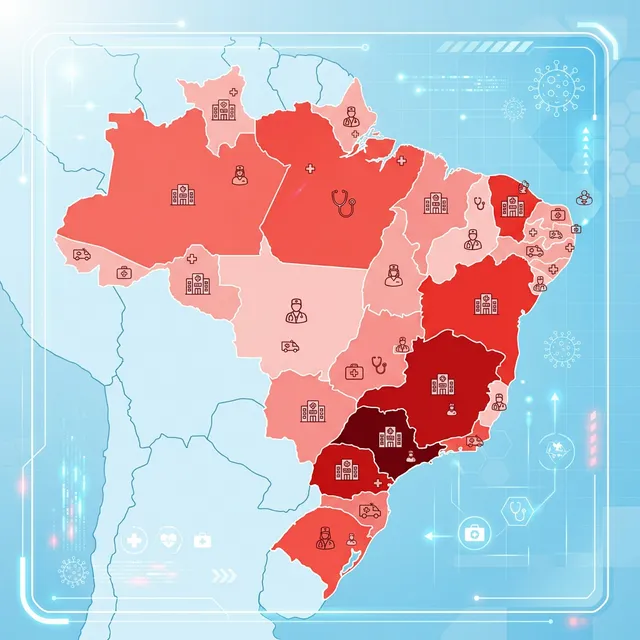
Geographic Distribution
São Paulo concentrates the absolute majority of cases, reflecting both the state's larger population and superior diagnostic capability:
| State | Confirmed Cases |
|---|---|
| São Paulo | 93 |
| Rio de Janeiro | 18 |
| Rondônia | 11 |
| Other states | 18 |
Comparison with 2025
An important point: the 2026 numbers are lower than those recorded in the same period of 2025. The Ministry of Health states that the current scenario does not constitute a crisis situation and that Brazil's public health system (SUS) is equipped for diagnosis, treatment, and monitoring of cases.
Symptoms: How to Identify Mpox
Mpox symptoms can vary in severity but generally follow a recognizable pattern. The incubation period is 5 to 21 days, with most symptoms appearing between 6 and 13 days after exposure.
Initial Symptoms (Prodromal Phase)
- Fever (generally above 38.5°C / 101.3°F)
- Intense headache
- Muscle and joint pain
- Extreme fatigue and weakness
- Swollen lymph nodes (lymphadenopathy) — a distinctive sign that differentiates Mpox from other dermatological conditions
- Chills and sweating
The Skin Rash (Eruptive Phase)
Generally 1 to 3 days after fever onset, skin lesions appear — the most characteristic symptom of the disease:
- Macules: flat red spots
- Papules: raised lesions
- Vesicles: blisters with clear fluid
- Pustules: blisters with pus
- Crusts: final healing phase
Lesions can appear anywhere on the body but are most common on the face, palms, soles, genital area, and oral mucosa. In the 2022 outbreak, genital and perianal lesions were particularly prevalent.
When to Seek Medical Care
Seek medical attention immediately if you experience:
- Unusual skin rashes, especially with blisters or pustules
- Fever associated with swollen lymph nodes
- Lesions in the genital or anal area
- History of contact with a confirmed or suspected case
Transmission: How Mpox Spreads
Mpox transmission occurs through close, direct physical contact with infected people, contaminated materials, or infected wild animals. Understanding the mechanisms of transmission is essential for adopting effective preventive measures.
Main Transmission Routes
- Skin-to-skin contact: direct touch with skin lesions, scabs, or body fluids from an infected person
- Intimate/sexual contact: the predominant route in the 2022-2023 outbreak, including contact during sexual intercourse
- Respiratory droplets: during prolonged, close contact (face to face), droplets can transmit the virus
- Contaminated materials: bed linens, towels, and other items that have been in contact with lesions
- Vertical transmission: from mother to child during pregnancy or childbirth
What Does NOT Transmit
- The virus is not airborne like COVID-19 under normal conditions
- Brief casual contact (such as a quick handshake or being in the same room) represents very low risk
- Food and water are not transmission vectors

Prevention and Vaccination
Preventive Measures
Mpox prevention involves a combination of individual and public health measures:
- Avoid contact with skin lesions or body fluids from infected people
- Hand hygiene: frequent washing with soap and water or hand sanitizer use
- Isolate materials: bed linens, towels, and personal items from infected people should be washed separately
- Use condoms: reduces transmission risk during sexual intercourse, although it does not completely eliminate the risk
- Partner communication: inform sexual partners about possible exposures
Mpox Vaccine
The Jynneos vaccine (also known as Imvanex in Europe) is the primary approved vaccine against Mpox. Originally developed against smallpox, it demonstrated an efficacy of 85% in preventing Mpox in clinical studies.
In Brazil, the vaccine was included in the public health system (SUS) for priority groups, including healthcare professionals, immunocompromised individuals, and those with high-risk exposure. The vaccination strategy follows WHO's recommendation for post-exposure vaccination in high-risk situations.
Treatment
Currently, Mpox treatment is primarily supportive — meaning focused on symptom relief. The antiviral tecovirimat (TPOXX) can be used in severe cases under emergency use authorization. Most patients recover completely within 2 to 4 weeks.
Is Mpox the New Pandemic? What Experts Say
This is a recurring question on social media and in doctors' offices. The experts' answer is clear: no, Mpox in its current form does not present the characteristics necessary for a pandemic on the level of COVID-19. However, vigilance is essential.
Why It's Not (Yet) a Pandemic
- Limited transmission: unlike COVID-19, Mpox requires direct physical contact, which significantly limits propagation speed
- Vaccine available: unlike SARS-CoV-2 in 2020, effective vaccines against Mpox already exist
- Established treatment: antivirals and clinical protocols are already developed
- Low lethality: Clade IIb, predominant in current outbreaks, has a fatality rate below 0.1%
Why Vigilance Is Necessary
- Viral recombination: the new variant combining clades Ib and IIb demonstrates the virus continues to evolve
- Vulnerable populations: immunocompromised individuals, children, and pregnant women face higher risks
- Access inequality: not all countries have equal access to vaccines and treatments
- Complacency: the greatest threat in public health is complacency — stopping monitoring when numbers appear low

The Global Scenario: Mpox Worldwide in 2026
Brazil is not alone in the fight against Mpox. The disease remains present on all continents, though with very different intensities.
Timeline of Key Events
| Date | Event |
|---|---|
| May 2022 | First global outbreak outside Africa — WHO declares emergency |
| Jul 2023 | WHO ends international emergency; global total exceeds 87,000 cases |
| Aug 2024 | WHO re-declares emergency due to Clade Ib outbreak in Central Africa |
| Dec 2025 | First detection of recombinant variant Ib+IIb in the United Kingdom |
| Jan 2026 | Recombinant variant confirmed in India |
| Feb 2026 | WHO officially documents the new recombinant strain |
| Mar 2026 | Brazil registers 140 confirmed cases in the year |
Africa: The Forgotten Epicenter
While Western countries discuss the new variant, the Democratic Republic of Congo remains the most affected country in the world by a considerable margin. In 2024 and 2025, Clade Ib caused thousands of deaths in the country, many of them among children under the age of five — a devastating statistic that was largely ignored by international media outlets for months on end. The humanitarian crisis in the DRC's eastern provinces, already battered by decades of armed conflict and displacement, was significantly worsened by the Mpox outbreak, with overwhelmed healthcare facilities struggling to provide basic treatment.
The inequality in vaccine access is stark and deeply troubling: while the United States and Europe continue to stockpile millions of Jynneos doses — many of which may never be administered — African countries depend on sparse, irregular donations and precarious cold-chain logistics to vaccinate their most vulnerable populations. The WHO has repeatedly and strongly criticized this disparity, issuing pointed warnings that the lack of disease control in Africa could result in new, more dangerous variants that will eventually reach the rest of the world — exactly as happened with COVID-19 and its successive variants of concern.
Europe and North America
In Europe, Mpox cases in 2026 remained relatively low compared to the 2022 peak, with most diagnoses concentrated in the United Kingdom, Germany, and France. Genomic surveillance across the continent has been elevated to its highest level following the detection of the recombinant variant. The European Centre for Disease Prevention and Control (ECDC) issued updated guidance in February 2026 recommending enhanced laboratory testing protocols.
The United States registered fewer than 500 Mpox cases between January and March 2026, a significant reduction from the 2022 outbreak that saw over 30,000 cases. However, the CDC (Centers for Disease Control and Prevention) increased the epidemiological alert level and expanded vaccination recommendations for healthcare workers and at-risk populations, reflecting continued caution about the evolving viral landscape.
Asia: The India Case
The detection of the recombinant variant in India in January 2026 triggered immediate global alarms among epidemiologists and public health officials. With a population exceeding 1.4 billion people and a healthcare system that faced enormous logistical and capacity challenges during the COVID-19 pandemic, the country is widely considered a critical inflection point for global epidemiological surveillance. Indian authorities responded swiftly with comprehensive contact tracing programs and rapid isolation of all identified cases, drawing on the institutional knowledge and infrastructure developed during the COVID-19 response.
Frequently Asked Questions (FAQ)
Is Mpox the same as smallpox?
No. Although they belong to the same viral family (Poxviridae), they are different viruses. Smallpox (caused by the Variola virus) was eradicated in 1980 and was far more lethal (30% mortality). Mpox has much lower lethality and generally milder symptoms.
Can I catch Mpox on public transportation?
The risk is extremely low. Mpox requires direct, prolonged physical contact for transmission. Sitting next to someone on a bus or subway does not represent significant risk, as long as there is no contact with skin lesions.
Does the smallpox vaccine protect against Mpox?
Yes. People vaccinated against smallpox before 1980 (when vaccination was discontinued) have partial immunity against Mpox, estimated at 85%. The Jynneos vaccine, available since 2019, was specifically developed to provide protection against both viruses with a superior safety profile.
Can children get Mpox?
Yes, although cases are less frequent in children outside Africa. In the Democratic Republic of Congo, Clade Ib disproportionately affected children with more severe outcomes. In Brazil, through March 2026, cases are predominantly in young adults.
How long does isolation last?
The recommended isolation period is until all skin lesions are completely healed and crusts have fallen off naturally. This generally takes 2 to 4 weeks, varying according to the severity of the individual case and the patient's overall immune health. During the isolation period, it is absolutely essential to avoid sharing personal items such as towels, razors, and eating utensils, and to keep bed linens and clothing separate from other household members.
Does Mpox leave scars?
In moderate to severe cases, Mpox can leave permanent scars, especially from facial lesions. Scarring depends on lesion severity and care during the active phase of the disease. Adequate skin hydration and avoiding scratching lesions can reduce scarring risk.
Conclusion: Vigilance Without Panic
Mpox in 2026 is not a reason for panic, but neither is it a reason for neglect. Brazil is in a relatively comfortable position — cases are lower than in 2025, there have been no deaths, and the public health system has response capacity. However, the emergence of the recombinant variant is a powerful reminder that viruses never stop evolving, and that complacency is the greatest ally of epidemics.
The best thing every citizen can do is stay informed through reliable sources, know the symptoms, adopt basic preventive measures, and, if belonging to a high-risk group, seek vaccination. Science has advanced enormously since the first cases in 2022, and we are much better prepared to face this virus than we were four years ago.
The most important lesson from Mpox is the same as every health crisis: constant vigilance is the price of public health. And while the world deals with wars, economic crises, and political polarization, health remains the most fundamental — and most fragile — right of all. Maintaining attention to warning signs, following medical guidance, and supporting public health systems are the best weapons we have against any viral threat.
What we cannot allow is for global inequality in access to vaccines and treatments to continue creating the perfect conditions for new variants to emerge. Mpox teaches us that in a hyperconnected world, no country is safe while all countries are not safe. Global health is, literally, everyone's problem.
If the COVID-19 pandemic taught us anything, it was that prior preparation makes all the difference between a controlled emergency and a catastrophe. In 2026, we have the advantage of being more prepared — we have vaccines, protocols, and genomic surveillance. What is often missing is the political will and individual awareness to use these tools before it's too late. Mpox is one more opportunity to prove that we learned from the past — and that we are capable of acting with intelligence, not with fear.
Sources and References

- Brazil Ministry of Health — Mpox Epidemiological Bulletin 2026
- Agência Brasil (EBC) — Mpox Cases in Brazil
- O Tempo — Mpox Case Updates
- UOL — Mpox in Brazil: Data and Prevention
- Metrópoles — Mpox Scenario 2026
- WHO — New Mpox Recombinant Variant
- Revista Abril — Recombinant Variant Ib+IIb
- Afya — Clinical Analysis of Recombinant Variant
- APM — São Paulo Medical Association
Last updated: March 10, 2026





