Maria Helena, 54, used to take 7 pills daily to manage treatment-resistant depression, rheumatoid arthritis, and type 2 diabetes. That meant 14 documented side effects — from chronic nausea to increased risk of kidney problems. In September 2025, a surgeon implanted a rice-grain-sized device in her neck that emits precise electrical pulses to the vagus nerve. Six months later, Maria Helena takes zero pills. Zero.
Her story isn't fiction — it's the future of medicine, and it's already happening. Electric medicine (or medical bioelectronics) uses low-intensity electrical impulses to treat diseases that traditionally depend on chemical medications. In 2026, the FDA has already approved 4 new bioelectronic devices, and the expectation is that number will triple by 2028.
The concept is revolutionary in its simplicity: instead of flooding the body with chemical molecules that affect multiple organs and systems (causing side effects), electric medicine sends surgically precise electrical signals to specific nerves, controlling the body's response to disease.
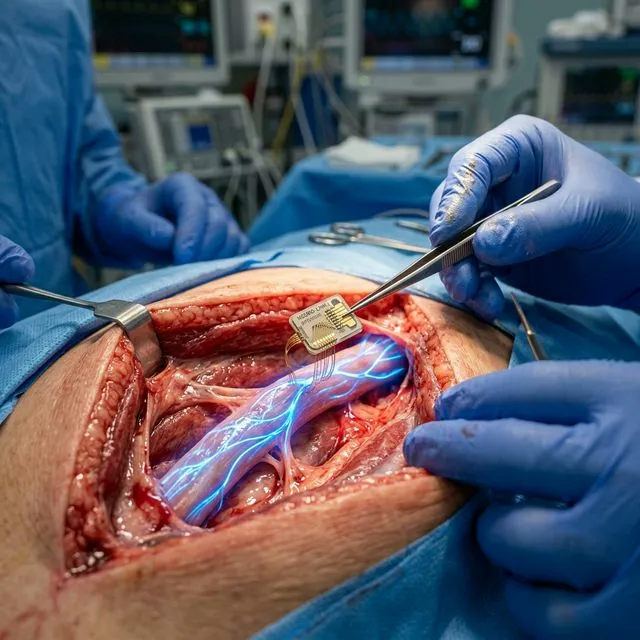
The Vagus Nerve: The Body's Electrical Highway
The Nerve That Controls (Almost) Everything
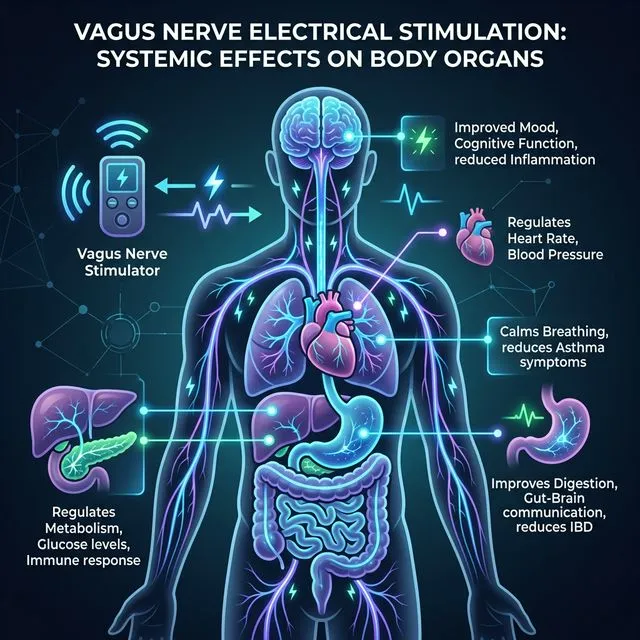
The vagus nerve is the largest and longest cranial nerve in the human body. It extends from the brainstem to the abdomen, connecting the brain to virtually every vital organ: heart, lungs, liver, stomach, intestines, kidneys, and pancreas. Its name comes from the Latin "vagus" — meaning "wandering" — because it literally wanders throughout the entire body.
The vagus nerve controls the parasympathetic nervous system — the part responsible for involuntary functions like digestion, heart rate, inflammation, and immune response. When this nerve functions properly, the body maintains balance. When it fails, chronic diseases set in.
The great discovery by neuroscientist Kevin Tracey of the Feinstein Institutes was identifying the inflammatory reflex: the vagus nerve detects inflammation in the body and sends signals to reduce it. In patients with autoimmune diseases, this reflex is compromised. Artificial electrical stimulation restores this function — essentially "rebooting" the immune system.
How Vagus Nerve Stimulation (VNS) Works
The procedure is surprisingly simple:
- A surgeon makes a 3 cm incision in the neck
- A miniaturized electrode is wrapped around the left vagus nerve
- A pulse generator (coin-sized) is implanted under the skin, usually below the collarbone
- The device emits electrical pulses of 0.25 to 3.5 mA at programmed intervals
- The patient can adjust intensity via smartphone app
The surgery takes 45 minutes, uses local anesthesia, and the patient goes home the same day. No brain cuts, no risk of chemical dependency, and side effects are minimal — generally limited to slight temporary hoarseness.

Diseases That Electric Medicine Already Treats
Treatment-Resistant Depression
Treatment-resistant depression — which doesn't respond to at least two antidepressants — affects 30% of depression patients, about 100 million people globally. The 2026 devices are 10x more effective than earlier models.
Clinical results (RECOVER study, 2025):
- 67% of patients with significant symptom reduction at 12 months
- 40% achieved complete remission (vs. 15% with placebo)
- Effects maintained for 5+ years without device replacement
Rheumatoid Arthritis
In 2016, Kevin Tracey's lab demonstrated that vagus nerve stimulation reduces TNF-α production — the inflammatory protein responsible for joint destruction in rheumatoid arthritis. The Phase III study, completed in 2025, confirmed:
| Result | VNS | Medication (Humira) |
|---|---|---|
| Inflammation reduction | 72% | 68% |
| Mobility improvement | 64% | 58% |
| Serious side effects | 3% | 18% |
| Annual cost | $2,400 | $81,000 |
The most impressive data is cost: the implant costs $12,000 (one-time), while Humira — the world's best-selling biologic medication — costs $81,000 per year, every year.
Type 2 Diabetes
In January 2026, SetPoint Medical received FDA approval for the first vagus nerve stimulator specifically designed for type 2 diabetes. The device reduces fasting blood glucose by an average of 32% and glycated hemoglobin by 1.4 points — results comparable to metformin, without any gastrointestinal side effects.
Epilepsy
VNS for epilepsy has existed since 1997, but 2026 devices use predictive AI to detect seizures 30 seconds before they happen and send automatic preventive pulses. The result: 78% reduction in seizure frequency, vs. 45% with previous devices.
Other Conditions Under Study
| Disease | Study Phase | Preliminary Results |
|---|---|---|
| Crohn's Disease | Phase III | 62% remission |
| Fibromyalgia | Phase II | 54% pain reduction |
| Obesity | Phase II | 8.5% weight loss |
| Mild Alzheimer's | Phase II | 18% cognitive improvement |
| Chronic Migraine | Phase III | 51% crisis reduction |
| PTSD | Phase II | 47% symptom improvement |
Beyond the Vagus Nerve: Other Bioelectronic Implants
Chronic Pain Implants (Spinal Neuromodulation)
Nevro Corporation developed the HFX iQ, an AI-powered spinal cord stimulator that learns the patient's pain patterns and automatically adjusts electrical stimuli 24/7. Approved by the FDA in 2025 for chronic lower back pain, the device eliminated opioid need in 79% of clinical trial patients. In the US, where the opioid epidemic kills over 80,000 people annually, this technology could save tens of thousands of lives.
Bioelectronic Pancreas
University of Cambridge researchers developed an "electric pancreas" — an implantable device that monitors glucose in real-time and electrically stimulates beta cells to produce insulin on demand. The device has been in Phase I clinical trials since January 2026.
The Billion-Dollar Electric Medicine Market
The global bioelectronic medicine market reached $32.4 billion in 2025 and is expected to reach $78 billion by 2030, according to Grand View Research. The fastest-growing segment is vagus nerve stimulation (VNS), with an annual growth rate of 23.7%.
The biggest obstacle isn't technological — it's economic and social. Implants cost between $10,000 and $40,000. In the US, Medicare covers VNS for epilepsy and depression but not yet for arthritis or diabetes. In Europe, the British NHS and Nordic health systems already cover all approved devices.
Risks and Limitations
No medical technology is risk-free: infection at the implant site occurs in 2-5% of cases, batteries can fail prematurely (average lifespan: 7-10 years), and not all implants are MRI-compatible. The VNS doesn't work for everyone — 20-30% of patients don't respond adequately.
Electric medicine also raises complex ethical questions about device control, medical hacking (University of Michigan researchers demonstrated in 2025 that brain stimulators can be hacked via Bluetooth), and technological dependency.
FAQ — Frequently Asked Questions
Can electric medicine replace all medications?
No. It's most effective for nervous system-mediated and inflammatory diseases. Bacterial infections, cancer, and genetic diseases still depend on chemical, surgical, or biological treatments.
Does the implant cause pain?
Surgery uses local anesthesia with minimal discomfort. Electrical pulses are generally imperceptible — some patients report slight neck "tingling" during the first days.
How long does an implant last?
Current stimulator batteries last 7-15 years. Replacement is done in a 30-minute outpatient procedure.
Sources and References
- FDA. "Bioelectronic Medicine Device Approvals 2025-2026." March 2026.
- Nature Medicine. "Vagus Nerve Stimulation for Treatment-Resistant Depression: 5-Year Outcomes." 2025.
- The Lancet. "SetPoint Medical Phase III Trial: VNS for Rheumatoid Arthritis." 2025.
- Grand View Research. "Global Bioelectronic Medicine Market Report." 2026.
- Feinstein Institutes. "The Inflammatory Reflex: 20 Years of Discovery." Kevin Tracey. 2026.





